|
- Korea–Thailand spine experts jointly lead advanced training on endoscopic spine surgery and lateral lumbar interbody fusion techniques
- Hands-on experience with Korean spine medical devices lays the foundation for advancing Asia's spine education hub
SEOUL, South Korea and BANGKOK, March 30, 2026 /PRNewswire/ -- CGBIO, a regenerative medicine-focused biomedical company led by CEO Hyun Seung Yu, announced on the 2nd that it recently hosted the "International Minimally Invasive Spine Surgery Education Forum (MEET THE MIS MASTERS: A Joint Korea–Thailand Forum)" at the Orthopaedic Learning Center, Faculty of Medicine, Siriraj Hospital in Bangkok, Thailand.
The forum was designed to provide leading spine surgeons across Asia with hands-on experience using the latest Korean-developed spine medical devices in Thailand, where demand for spinal surgery is rapidly increasing due to population aging and the growing prevalence of spinal disorders.
Beyond academic exchange, the forum was particularly meaningful as it helped establish a foundation for providing minimally invasive spine surgery to local patients—reducing surgical incisions and enabling faster recovery.
The event was co-hosted by The Catholic University of Korea and Chulalongkorn University, with support from the Ministry of Health and Welfare of Korea, the Korea Health Industry Development Institute (KHIDI), and Seongnam City.
More than 50 spine surgeons from eight Asian countries, including Korea and Thailand, participated, and the course directors were Professor Jin Sung Kim of Seoul St. Mary's Hospital, The Catholic University of Korea, and Professor Wicharn Yingsakmongkol of Chulalongkorn University.
The two-day program consisted of lectures on endoscopic spine surgery (biportal and uniportal techniques) and Oblique Lumbar Interbody Fusion (OLIF), cadaver-based hands-on training simulating real clinical environments, case studies, and clinical discussions.
Participants were divided into small groups to practice advanced techniques firsthand, share clinical application experiences, and strengthen academic and professional networks.
Through this initiative, the forum facilitated the dissemination of the latest minimally invasive spine surgery knowledge, strengthened collaboration and academic networks between Korean and Thai experts, and laid the groundwork for future joint research initiatives and procedural standardization.
CGBIO operated two of the six cadaver training stations and led hands-on education focused on biportal endoscopic decompression and interbody fusion.
The sessions were instructed by Professor Yong San Koh of Kyungpook National University Hospital, Director Sang Hyun Han of Asan Chungmu Hospital Spine Center, Professor Asrafi Rizki Gatam of Fatmawati General Hospital (Indonesia), and Professor Javier of Hospital Angeles Centro Sur (Mexico).
Participants directly used CGBIO products, including the bone graft substitute NOVOSIS, the expandable cage ExCender, and the minimally invasive screw system Colonnade, allowing them to assess firsthand the safety and competitiveness of Korean spine medical devices.
The hands-on training is also expected to enhance participants' surgical proficiency and clinical safety.
Professor Jin Sung Kim of Seoul St. Mary's Hospital, The Catholic University of Korea, stated, "Since 2022, the Korea Medical Device Education and Training Support Center initiative has steadily evolved through the development of educational content, clinical validation of surgical products, and professional training programs, as well as expanded domestic academic exchange. Building on the experience and expertise accumulated over the years, it is particularly meaningful to now actively support Korean companies in strengthening their competitiveness and growth in overseas markets. We will continue to provide academic support to facilitate their global expansion and export growth."
Hyun Seung Yu, CEO of CGBIO, stated, "This forum was meaningful in that it went beyond technical training and provided overseas spine surgeons with direct experience using Korean spine medical devices. The fact that technologies developed in Korea were applied in real surgical training settings and recognized for their effectiveness by medical professionals serves as clear evidence that Korean medical devices can meaningfully contribute to improving patient outcomes across Asia."
He added, "Building on this experience, CGBIO will expand international academic exchange and establish a global education network, positioning itself as a trusted spine surgery education hub and a leading representative of Korean medical devices not only in Asia but worldwide."
- Korea–Thailand spine experts jointly lead advanced training on endoscopic spine surgery and lateral lumbar interbody fusion techniques
- Hands-on experience with Korean spine medical devices lays the foundation for advancing Asia's spine education hub
SEOUL, South Korea and BANGKOK, March 30, 2026 /PRNewswire/ -- CGBIO, a regenerative medicine-focused biomedical company led by CEO Hyun Seung Yu, announced on the 2nd that it recently hosted the "International Minimally Invasive Spine Surgery Education Forum (MEET THE MIS MASTERS: A Joint Korea–Thailand Forum)" at the Orthopaedic Learning Center, Faculty of Medicine, Siriraj Hospital in Bangkok, Thailand.
The forum was designed to provide leading spine surgeons across Asia with hands-on experience using the latest Korean-developed spine medical devices in Thailand, where demand for spinal surgery is rapidly increasing due to population aging and the growing prevalence of spinal disorders.
Beyond academic exchange, the forum was particularly meaningful as it helped establish a foundation for providing minimally invasive spine surgery to local patients—reducing surgical incisions and enabling faster recovery.
The event was co-hosted by The Catholic University of Korea and Chulalongkorn University, with support from the Ministry of Health and Welfare of Korea, the Korea Health Industry Development Institute (KHIDI), and Seongnam City.
More than 50 spine surgeons from eight Asian countries, including Korea and Thailand, participated, and the course directors were Professor Jin Sung Kim of Seoul St. Mary's Hospital, The Catholic University of Korea, and Professor Wicharn Yingsakmongkol of Chulalongkorn University.
The two-day program consisted of lectures on endoscopic spine surgery (biportal and uniportal techniques) and Oblique Lumbar Interbody Fusion (OLIF), cadaver-based hands-on training simulating real clinical environments, case studies, and clinical discussions.
Participants were divided into small groups to practice advanced techniques firsthand, share clinical application experiences, and strengthen academic and professional networks.
Through this initiative, the forum facilitated the dissemination of the latest minimally invasive spine surgery knowledge, strengthened collaboration and academic networks between Korean and Thai experts, and laid the groundwork for future joint research initiatives and procedural standardization.
CGBIO operated two of the six cadaver training stations and led hands-on education focused on biportal endoscopic decompression and interbody fusion.
The sessions were instructed by Professor Yong San Koh of Kyungpook National University Hospital, Director Sang Hyun Han of Asan Chungmu Hospital Spine Center, Professor Asrafi Rizki Gatam of Fatmawati General Hospital (Indonesia), and Professor Javier of Hospital Angeles Centro Sur (Mexico).
Participants directly used CGBIO products, including the bone graft substitute NOVOSIS, the expandable cage ExCender, and the minimally invasive screw system Colonnade, allowing them to assess firsthand the safety and competitiveness of Korean spine medical devices.
The hands-on training is also expected to enhance participants' surgical proficiency and clinical safety.
Professor Jin Sung Kim of Seoul St. Mary's Hospital, The Catholic University of Korea, stated, "Since 2022, the Korea Medical Device Education and Training Support Center initiative has steadily evolved through the development of educational content, clinical validation of surgical products, and professional training programs, as well as expanded domestic academic exchange. Building on the experience and expertise accumulated over the years, it is particularly meaningful to now actively support Korean companies in strengthening their competitiveness and growth in overseas markets. We will continue to provide academic support to facilitate their global expansion and export growth."
Hyun Seung Yu, CEO of CGBIO, stated, "This forum was meaningful in that it went beyond technical training and provided overseas spine surgeons with direct experience using Korean spine medical devices. The fact that technologies developed in Korea were applied in real surgical training settings and recognized for their effectiveness by medical professionals serves as clear evidence that Korean medical devices can meaningfully contribute to improving patient outcomes across Asia."
He added, "Building on this experience, CGBIO will expand international academic exchange and establish a global education network, positioning itself as a trusted spine surgery education hub and a leading representative of Korean medical devices not only in Asia but worldwide."
** This press release is distributed by PR Newswire through automated distribution system, for which the client assumes full responsibility. **

CGBIO Showcases Minimally Invasive Spine Surgery Techniques in Thailand: "Smaller Incisions, Faster Recovery"
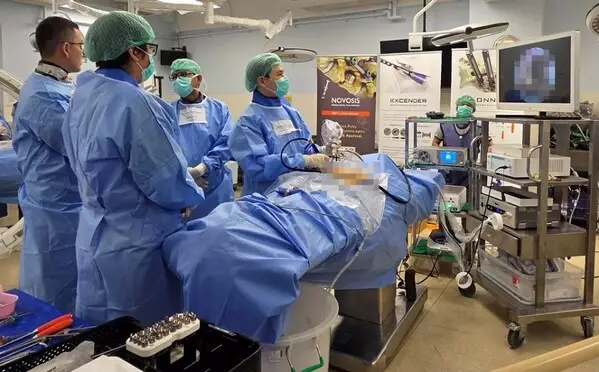
CGBIO Showcases Minimally Invasive Spine Surgery Techniques in Thailand: "Smaller Incisions, Faster Recovery"
|
Honouring 35 patients who stand as inspiring examples of resilience, underscoring the long-term success of organ transplantation
SINGAPORE, March 30, 2026 /PRNewswire/ -- For transplant recipients, reaching the 25-year mark is a significant achievement. According to international statistics, a deceased donor kidney lasts about 8 to 12 years, while a living donor kidney transplant typically lasts 15 to 20 years on average [1]; liver transplants may last from 10 to 20 years[2], though sometimes longer. Historically, the success rates of kidney transplantation before 2000 were much lower than they are today. With advances in immunosuppression and healthcare, success rates are much better.
Today, at the National University Centre for Organ Transplantation (NUCOT), average survivals for adult deceased donor and living donor kidney transplants are 15 and 31 years respectively. Achieving these outcomes that surpass international benchmarks by two- to four-fold is only possible with holistic and multidisciplinary care that can be delivered at centres such as NUCOT.
NUCOT has organised an evening of celebration as a tribute to a remarkable group of individuals who have reached 25 years of life or more after a kidney or liver transplant. The event will bring together 35 such patients, making it one of the largest gatherings of long-term transplant survivors of its kind, alongside their living donors, family members and healthcare professionals. The occasion stands as a testament to the fortitude of these transplant recipients and to NUCOT's longstanding commitment to delivering comprehensive, top-quality transplant and post-transplant care. It also honours their families, medical teams and the generosity of organ donors whose gifts have given recipients the chance to enjoy decades of renewed life.
Professor A Vathsala, Director of NUCOT, said: "Reaching 25 years after an organ transplant is an extraordinary milestone, and it is never an easy journey. Every patient who stands here today has not only endured the physical demands of complex medical challenges and the emotional weight of uncertainty, but also repeated treatments and lifelong adjustments. To see them living, thriving and dreaming a quarter century on is a profound reminder of why we do what we do at NUCOT."
Strong outcomes backed by comprehensive, multidisciplinary care
Transplantation is a miracle of modern medicine but sustaining a transplanted organ over decades remains medically challenging. The most important medical problem faced by organ transplant recipients is rejection which occurs when the patient's immune system perceives the transplanted organ as a foreign invader and attempts to attack and destroy it. Transplant recipients must therefore take lifelong immunosuppressant medications to prevent rejection. However, these immunosuppressive medications also prevent the recipient's immune system from attacking other invaders such as bacteria or viruses, therefore increasing the patient's risk of infections.
Immunosuppressive medications can also give rise to other complications such as diabetes, high blood pressure and kidney impairment. Avoiding rejection on the one hand, and infections and medication-related complications on the other, is a fine balancing act. It is only if this balancing act is done well that outstanding results can be achieved, and transplant recipients are able to reach this milestone of 25 years and beyond.
NUCOT has incorporated the latest advances in transplant medicine such as advanced tissue typing and antibody assessment methodologies, molecular biological approaches to assess infections and rejection, the latest perfusion technologies to better preserve organs, and modern methods to perform complex procedures such as blood group incompatible transplants. Beyond technology, it also has a multidisciplinary team that ensures holistic patient management, including tailored immunosuppression protocols, close long-term follow-up for life after transplant, as well as education on medication adherence and lifestyle modifications post-transplants.
The centre's 10-year statistics show that its clinical outcomes are better than or comparable with international benchmarks. For instance, the 10-year survival rate for adult patients who underwent living donor kidney transplant is 90 per cent, compared to 82.7 per cent in the United States and 86 per cent in Australia/New Zealand. For adult patients who underwent living donor liver transplant, the 10-year survival rate is 78 per cent, compared to 67.9 per cent in the US and 61 per cent in Europe.
In paediatric transplant, the organ needs to last through a child's developmental years and well into adulthood to allow the individual to live a productive and fulfilling life. Indeed, NUCOT has delivered even better survival at 10 years for paediatric organ recipients in comparison to counterparts in the US and Europe. NUCOT's paediatric kidney patient survival at 10 years is 92.9 per cent, compared to 90.5 per cent in the US and 74 per cent in Europe; the centre's paediatric liver patient survival is 82.2 per cent, while it is 70 per cent in the US and 75.8 per cent in Europe.
Twenty-year survival benchmarks are less easily available. At NUCOT, patient survival for adult kidney transplant at 20 years is 76 per cent for living donor transplants (vs 66 per cent based on data from the Australia-New Zealand registry) and 67 per cent for deceased donor transplants (vs 50 per cent from the New Zealand registry). That so many at NUCOT have thrived for more than two decades speaks to both their determination and the quality of care they have received.
Lives rebuilt across decades
Dr Leong Sai Fan, a 70-year-old retiree, received a kidney from his wife Mdm Quek Seow Chiang who donated her kidney to him in 1997. At the time, a transplant between genetically unrelated individuals required special approval, before legislative changes in 2004 allowed such transplants more widely.
He said: "My transplanted kidney has lasted 29 years. It gave me a new lease of life and was a gift made possible by my wife who could not bear to see me suffer. As part of the early generation who benefited from living donor transplants, I was able to continue working, watch our children grow, and now enjoy being a grandfather of four. I'm deeply grateful to my wife, and to the doctors and transplant coordinators who have cared for me over the years. They feel more like friends now in many ways."
Another long-term transplant recipient is Mdm Leong Kwai Sin, who at 41 years post-transplant is one of NUCOT's longest surviving patients. Now 69, Mdm Leong had undergone a kidney transplant due to kidney failure in 1985. She said: "It has been more than four decades since my kidney transplant, and every day since has been a gift. I am especially grateful to Professor Vathsala, who not only cared for me medically but supported me wholeheartedly when I hoped to start a family. She tailored my post‑transplant care to make sure I was healthy enough to conceive, and I always felt safe under her guidance. Tonight's celebration reminds me how far we've come and how deeply the care from NUCOT has shaped my life."
In a separate case, Ms Tay (who preferred not to be fully named) was only around three years old when she had a liver transplant in 1996, making her the youngest liver transplant recipient in Singapore at the time. She was born with biliary atresia, a rare condition affecting newborns where the bile duct is blocked or did not develop properly.
Now in her early 30s, she recounts: "Receiving a liver transplant 30 years ago allowed me to live on and have a normal childhood, which I would otherwise not have had. Years later, I was also able to pursue tertiary education overseas. Since then, I could work full-time and pursue graduate studies. As such, I am deeply grateful for this gift of life and the ongoing care from the NUCOT team that made it possible."
A leading transplant centre with over 50 years of experience
Faculty from the National University of Singapore and National University Hospital have been at the forefront of advances in transplantation for over 50 years. Professor Khoo Oon Teik from the University Department of Medicine established a haemodialysis unit at the Outram campus, laying the groundwork for a kidney transplant programme. Professor Chan Kong Thoe from the University Department of Surgery performed the first cadaveric kidney transplant in Singapore on 8 July 1970. The first living donor kidney transplant in Singapore was performed in 1976 by Professors Ong Siew Chey, Foong Weng Cheong and Abu Rauff, all from the University Department of Surgery.
Notably, this year marks the 50th anniversary of the very first living donor kidney transplant in Singapore and NUCOT is privileged to have Professor Abu Rauff grace this celebration.
In 1985, the University Departments of Medicine and Surgery moved from the Outram campus to their present location at the National University Hospital. Under the leadership of Associate Professor Evan Lee, Professor Prabhakaran Krishnan and Professor Yap Hui Kim, the transplant programmes have grown from strength to strength. At NUH, Singapore's first paediatric kidney transplant was performed in February 1989, the first liver transplant in September 1990, and the first simultaneous kidney-pancreas transplant in 2012.
Since 1987, NUCOT has successfully carried out over 900 kidney and 500 liver transplants on both adult and paediatric patients. It remains Singapore's only centre performing paediatric solid organ transplants and has carried out over 100 paediatric kidney transplants and 150 paediatric liver transplants.
NUCOT was officially created in 2012 to bring together healthcare professionals in the kidney, liver, paediatric and pancreas programmes to advance care for organ transplant recipients. NUCOT's model of care is driven by a diverse team of transplant physicians, surgeons, nurses, pharmacists, allied health professionals and counsellors who work closely to provide holistic, long-term support for transplant patients and their families.
NUCOT also serves as a key hub for clinical training and research in Southeast Asia. Its commitment to education, innovation, and regional collaboration enables the centre to provide advanced treatments and foster expertise in organ donation and transplantation.
As NUCOT marks the 25-year milestone of post-transplant life with its patients, it remains committed to advancing transplant medicine so as to improve patient outcomes and transform patient lives after transplantation.
Chinese Glossary
| National University Centre for Organ Transplantation (NUCOT) | 国大医院器官移植中心 |
| Professor A Vathsala Director, NUCOT Head & Senior Consultant, Department of Medicine National University Hospital | A Vathsala教授 国大医院器官移植中心主任 内科部门主任及高级顾问医生 国立大学医院 |
| Associate Professor Evan Lee Emeritus Consultant Division of Nephrology Department of Medicine National University Hospital | Evan Lee 副教授 荣誉顾问医生 肾脏科 国立大学医院 |
| Emeritus Professor Prabhakaran Krishnan Emeritus Consultant Department of Paediatric Surgery Khoo Teck Puat - National University Children's Medical Institute National University Hospital | Prabhakaran Krishnan荣誉教授 荣誉顾问医生 小儿外科 邱德拔-国立大学儿童医疗中心 国立大学医院 |
| Professor Yap Hui Kim Medical Director & Emeritus Consultant Paediatric Kidney Transplantation Programme National University Centre for Organ Transplantation National University Hospital | 叶慧钦教授 内科主任兼荣誉顾问医生 小儿肾脏移植计划 国大医院器官移植中心 国立大学医院 |
About the National University Hospital (NUH)
The National University Hospital (NUH) is Singapore's leading university hospital. While the hospital at Kent Ridge first received its patients on 24 June 1985, our legacy started from 1905, the date of the founding of what is today the NUS Yong Loo Lin School of Medicine. NUH is the principal teaching hospital of the medical school.
Our unique identity as a university hospital is a key attraction for healthcare professionals who aspire to do more than practise tertiary medical care. We offer an environment where research and teaching are an integral part of medicine, and continue to shape medicine and transform care for the community we care for.
We are an academic medical centre with over 1,200 beds, serving more than one million patients a year with over 50 medical, surgical and dental specialties. NUH is the only public and not-for-profit hospital in Singapore to provide trusted care for adults, women and children under one roof, including the only paediatric kidney and liver transplant programme in the country.
The NUH is a key member of the National University Health System (NUHS), one of three public healthcare clusters in Singapore. For more information, visit www.nuh.com.sg
Follow us on
Facebook | Instagram | LinkedIn | TikTok | YouTube
Honouring 35 patients who stand as inspiring examples of resilience, underscoring the long-term success of organ transplantation
SINGAPORE, March 30, 2026 /PRNewswire/ -- For transplant recipients, reaching the 25-year mark is a significant achievement. According to international statistics, a deceased donor kidney lasts about 8 to 12 years, while a living donor kidney transplant typically lasts 15 to 20 years on average [1]; liver transplants may last from 10 to 20 years[2], though sometimes longer. Historically, the success rates of kidney transplantation before 2000 were much lower than they are today. With advances in immunosuppression and healthcare, success rates are much better.
Today, at the National University Centre for Organ Transplantation (NUCOT), average survivals for adult deceased donor and living donor kidney transplants are 15 and 31 years respectively. Achieving these outcomes that surpass international benchmarks by two- to four-fold is only possible with holistic and multidisciplinary care that can be delivered at centres such as NUCOT.
NUCOT has organised an evening of celebration as a tribute to a remarkable group of individuals who have reached 25 years of life or more after a kidney or liver transplant. The event will bring together 35 such patients, making it one of the largest gatherings of long-term transplant survivors of its kind, alongside their living donors, family members and healthcare professionals. The occasion stands as a testament to the fortitude of these transplant recipients and to NUCOT's longstanding commitment to delivering comprehensive, top-quality transplant and post-transplant care. It also honours their families, medical teams and the generosity of organ donors whose gifts have given recipients the chance to enjoy decades of renewed life.
Professor A Vathsala, Director of NUCOT, said: "Reaching 25 years after an organ transplant is an extraordinary milestone, and it is never an easy journey. Every patient who stands here today has not only endured the physical demands of complex medical challenges and the emotional weight of uncertainty, but also repeated treatments and lifelong adjustments. To see them living, thriving and dreaming a quarter century on is a profound reminder of why we do what we do at NUCOT."
Strong outcomes backed by comprehensive, multidisciplinary care
Transplantation is a miracle of modern medicine but sustaining a transplanted organ over decades remains medically challenging. The most important medical problem faced by organ transplant recipients is rejection which occurs when the patient's immune system perceives the transplanted organ as a foreign invader and attempts to attack and destroy it. Transplant recipients must therefore take lifelong immunosuppressant medications to prevent rejection. However, these immunosuppressive medications also prevent the recipient's immune system from attacking other invaders such as bacteria or viruses, therefore increasing the patient's risk of infections.
Immunosuppressive medications can also give rise to other complications such as diabetes, high blood pressure and kidney impairment. Avoiding rejection on the one hand, and infections and medication-related complications on the other, is a fine balancing act. It is only if this balancing act is done well that outstanding results can be achieved, and transplant recipients are able to reach this milestone of 25 years and beyond.
NUCOT has incorporated the latest advances in transplant medicine such as advanced tissue typing and antibody assessment methodologies, molecular biological approaches to assess infections and rejection, the latest perfusion technologies to better preserve organs, and modern methods to perform complex procedures such as blood group incompatible transplants. Beyond technology, it also has a multidisciplinary team that ensures holistic patient management, including tailored immunosuppression protocols, close long-term follow-up for life after transplant, as well as education on medication adherence and lifestyle modifications post-transplants.
The centre's 10-year statistics show that its clinical outcomes are better than or comparable with international benchmarks. For instance, the 10-year survival rate for adult patients who underwent living donor kidney transplant is 90 per cent, compared to 82.7 per cent in the United States and 86 per cent in Australia/New Zealand. For adult patients who underwent living donor liver transplant, the 10-year survival rate is 78 per cent, compared to 67.9 per cent in the US and 61 per cent in Europe.
In paediatric transplant, the organ needs to last through a child's developmental years and well into adulthood to allow the individual to live a productive and fulfilling life. Indeed, NUCOT has delivered even better survival at 10 years for paediatric organ recipients in comparison to counterparts in the US and Europe. NUCOT's paediatric kidney patient survival at 10 years is 92.9 per cent, compared to 90.5 per cent in the US and 74 per cent in Europe; the centre's paediatric liver patient survival is 82.2 per cent, while it is 70 per cent in the US and 75.8 per cent in Europe.
Twenty-year survival benchmarks are less easily available. At NUCOT, patient survival for adult kidney transplant at 20 years is 76 per cent for living donor transplants (vs 66 per cent based on data from the Australia-New Zealand registry) and 67 per cent for deceased donor transplants (vs 50 per cent from the New Zealand registry). That so many at NUCOT have thrived for more than two decades speaks to both their determination and the quality of care they have received.
Lives rebuilt across decades
Dr Leong Sai Fan, a 70-year-old retiree, received a kidney from his wife Mdm Quek Seow Chiang who donated her kidney to him in 1997. At the time, a transplant between genetically unrelated individuals required special approval, before legislative changes in 2004 allowed such transplants more widely.
He said: "My transplanted kidney has lasted 29 years. It gave me a new lease of life and was a gift made possible by my wife who could not bear to see me suffer. As part of the early generation who benefited from living donor transplants, I was able to continue working, watch our children grow, and now enjoy being a grandfather of four. I'm deeply grateful to my wife, and to the doctors and transplant coordinators who have cared for me over the years. They feel more like friends now in many ways."
Another long-term transplant recipient is Mdm Leong Kwai Sin, who at 41 years post-transplant is one of NUCOT's longest surviving patients. Now 69, Mdm Leong had undergone a kidney transplant due to kidney failure in 1985. She said: "It has been more than four decades since my kidney transplant, and every day since has been a gift. I am especially grateful to Professor Vathsala, who not only cared for me medically but supported me wholeheartedly when I hoped to start a family. She tailored my post‑transplant care to make sure I was healthy enough to conceive, and I always felt safe under her guidance. Tonight's celebration reminds me how far we've come and how deeply the care from NUCOT has shaped my life."
In a separate case, Ms Tay (who preferred not to be fully named) was only around three years old when she had a liver transplant in 1996, making her the youngest liver transplant recipient in Singapore at the time. She was born with biliary atresia, a rare condition affecting newborns where the bile duct is blocked or did not develop properly.
Now in her early 30s, she recounts: "Receiving a liver transplant 30 years ago allowed me to live on and have a normal childhood, which I would otherwise not have had. Years later, I was also able to pursue tertiary education overseas. Since then, I could work full-time and pursue graduate studies. As such, I am deeply grateful for this gift of life and the ongoing care from the NUCOT team that made it possible."
A leading transplant centre with over 50 years of experience
Faculty from the National University of Singapore and National University Hospital have been at the forefront of advances in transplantation for over 50 years. Professor Khoo Oon Teik from the University Department of Medicine established a haemodialysis unit at the Outram campus, laying the groundwork for a kidney transplant programme. Professor Chan Kong Thoe from the University Department of Surgery performed the first cadaveric kidney transplant in Singapore on 8 July 1970. The first living donor kidney transplant in Singapore was performed in 1976 by Professors Ong Siew Chey, Foong Weng Cheong and Abu Rauff, all from the University Department of Surgery.
Notably, this year marks the 50th anniversary of the very first living donor kidney transplant in Singapore and NUCOT is privileged to have Professor Abu Rauff grace this celebration.
In 1985, the University Departments of Medicine and Surgery moved from the Outram campus to their present location at the National University Hospital. Under the leadership of Associate Professor Evan Lee, Professor Prabhakaran Krishnan and Professor Yap Hui Kim, the transplant programmes have grown from strength to strength. At NUH, Singapore's first paediatric kidney transplant was performed in February 1989, the first liver transplant in September 1990, and the first simultaneous kidney-pancreas transplant in 2012.
Since 1987, NUCOT has successfully carried out over 900 kidney and 500 liver transplants on both adult and paediatric patients. It remains Singapore's only centre performing paediatric solid organ transplants and has carried out over 100 paediatric kidney transplants and 150 paediatric liver transplants.
NUCOT was officially created in 2012 to bring together healthcare professionals in the kidney, liver, paediatric and pancreas programmes to advance care for organ transplant recipients. NUCOT's model of care is driven by a diverse team of transplant physicians, surgeons, nurses, pharmacists, allied health professionals and counsellors who work closely to provide holistic, long-term support for transplant patients and their families.
NUCOT also serves as a key hub for clinical training and research in Southeast Asia. Its commitment to education, innovation, and regional collaboration enables the centre to provide advanced treatments and foster expertise in organ donation and transplantation.
As NUCOT marks the 25-year milestone of post-transplant life with its patients, it remains committed to advancing transplant medicine so as to improve patient outcomes and transform patient lives after transplantation.
[1] Source: National Kidney Foundation, https://www.kidney.org/kidney-topics/kidney-transplant
[2] Source: British Medical Journal, https://www.bmj.com/content/bmj/379/bmj.o2541.full.pdf
Chinese Glossary
| National University Centre for Organ Transplantation (NUCOT) | 国大医院器官移植中心 |
| Professor A Vathsala Director, NUCOT Head & Senior Consultant, Department of Medicine National University Hospital | A Vathsala教授 国大医院器官移植中心主任 内科部门主任及高级顾问医生 国立大学医院 |
| Associate Professor Evan Lee Emeritus Consultant Division of Nephrology Department of Medicine National University Hospital | Evan Lee 副教授 荣誉顾问医生 肾脏科 国立大学医院 |
| Emeritus Professor Prabhakaran Krishnan Emeritus Consultant Department of Paediatric Surgery Khoo Teck Puat - National University Children's Medical Institute National University Hospital | Prabhakaran Krishnan荣誉教授 荣誉顾问医生 小儿外科 邱德拔-国立大学儿童医疗中心 国立大学医院 |
| Professor Yap Hui Kim Medical Director & Emeritus Consultant Paediatric Kidney Transplantation Programme National University Centre for Organ Transplantation National University Hospital | 叶慧钦教授 内科主任兼荣誉顾问医生 小儿肾脏移植计划 国大医院器官移植中心 国立大学医院 |
National University Centre for Organ Transplantation (NUCOT)
国大医院器官移植中心
Professor A Vathsala
Director, NUCOT
Head & Senior Consultant, Department of Medicine
National University Hospital
A Vathsala教授
国大医院器官移植中心主任
内科部门主任及高级顾问医生
国立大学医院
Associate Professor Evan Lee
Emeritus Consultant
Division of Nephrology
Department of Medicine
National University Hospital
Evan Lee 副教授
荣誉顾问医生
肾脏科
国立大学医院
Emeritus Professor Prabhakaran Krishnan
Emeritus Consultant
Department of Paediatric Surgery
Khoo Teck Puat - National University Children's Medical Institute
National University Hospital
Prabhakaran Krishnan荣誉教授
荣誉顾问医生
小儿外科
邱德拔-国立大学儿童医疗中心
国立大学医院
Professor Yap Hui Kim
Medical Director & Emeritus Consultant
Paediatric Kidney Transplantation Programme
National University Centre for Organ Transplantation
National University Hospital
叶慧钦教授
内科主任兼荣誉顾问医生
小儿肾脏移植计划
国大医院器官移植中心
国立大学医院
About the National University Hospital (NUH)
The National University Hospital (NUH) is Singapore's leading university hospital. While the hospital at Kent Ridge first received its patients on 24 June 1985, our legacy started from 1905, the date of the founding of what is today the NUS Yong Loo Lin School of Medicine. NUH is the principal teaching hospital of the medical school.
Our unique identity as a university hospital is a key attraction for healthcare professionals who aspire to do more than practise tertiary medical care. We offer an environment where research and teaching are an integral part of medicine, and continue to shape medicine and transform care for the community we care for.
We are an academic medical centre with over 1,200 beds, serving more than one million patients a year with over 50 medical, surgical and dental specialties. NUH is the only public and not-for-profit hospital in Singapore to provide trusted care for adults, women and children under one roof, including the only paediatric kidney and liver transplant programme in the country.
The NUH is a key member of the National University Health System (NUHS), one of three public healthcare clusters in Singapore. For more information, visit www.nuh.com.sg
Follow us on
Facebook | Instagram | LinkedIn | TikTok | YouTube
** This press release is distributed by PR Newswire through automated distribution system, for which the client assumes full responsibility. **

CELEBRATING 25 YEARS AND BEYOND OF LIFE AFTER ORGAN TRANSPLANTATION AT THE NATIONAL UNIVERSITY CENTRE FOR ORGAN TRANSPLANTATION












