Puts a whole new perspective to "blood, sweat and tears"...
It was reported that this 11-year-old Vietnamese girl was revising for an exam when she suddenly started "sweating blood", in what is later speculated to be an exceptionally uncommon condition called "hematohidrosis".
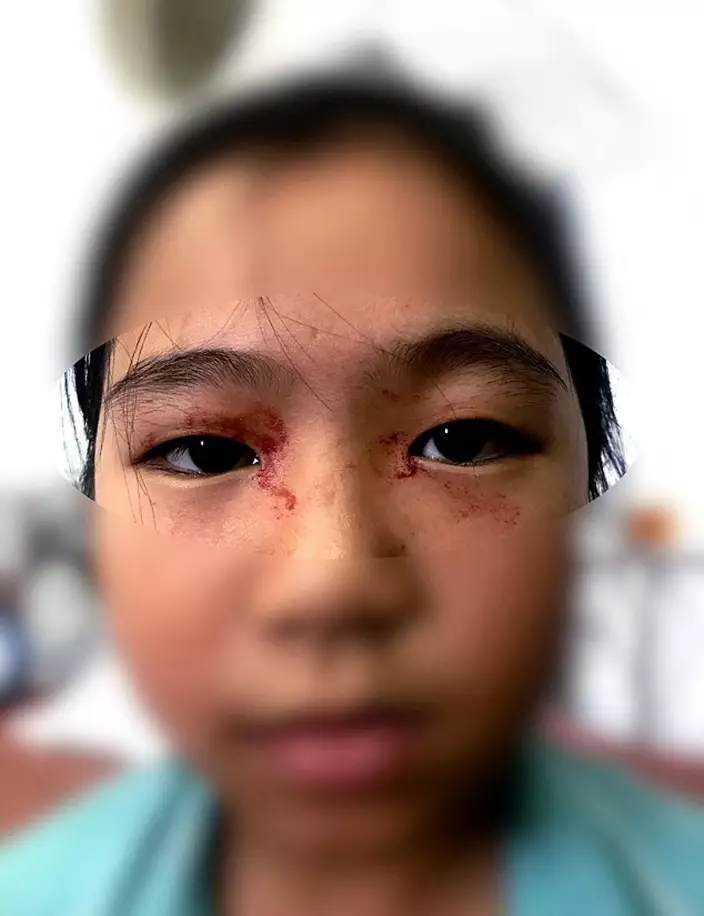
Online image
The girl, from Dak Doa in the province of Jal., was found to have blood oozing out of her face when she was preparing for a school examination a few months ago. Doctors initially diagnosed her with a skin infection, but because her condition did not improve even after a round of treatment, the doctors realised it wasn't as they originally thought.
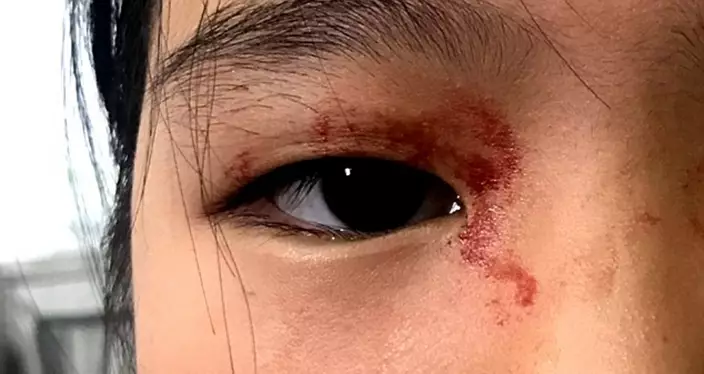
Online image
Doctors at the National Leprosy Dermatology Hospital believes that the girl suffers from "hematohidrosis", an extremely rare disorder that only affects 1 out of 10 million people, and as such, the medical community is not very well versed in the disorder or the remedies for it.
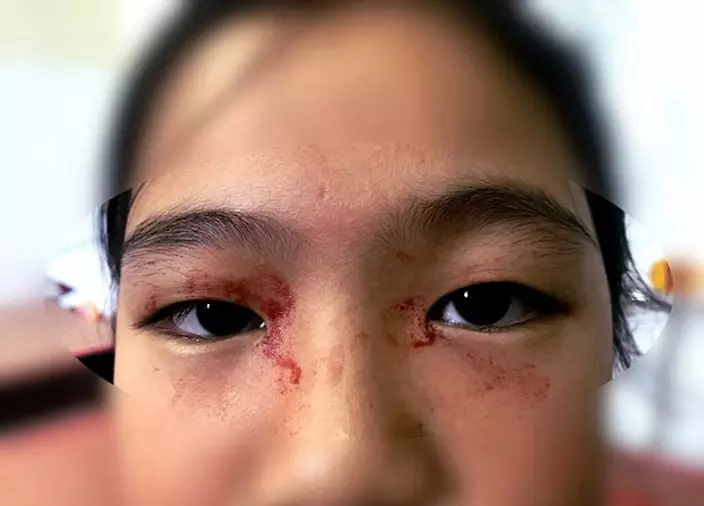
Online image
The only information they know is that the sufferers of hematohidrosis have 20 times the average amount of adrenaline in their bloodstream when under stress, which may contribute to huge increases in blood pressure, which may cause capillaries in the skin to burst, causing haemorrhage and the peculiar phenomenon of "sweating blood".
Online image
Wu Junying, the dean of the National Maternal Dermatology Hospital, pointed out that patients with hematohidrosis will "sweat blood" when under emotional stress, and that treatment for this rare disorder is not easy. at present, they can only focus on symptoms and help patients with their stress and anxiety. They will be prescribed with vitamin C, antidepressants and Propranolol, along with some other drugs.
Doctor Wu said that hematohidrosis does not shorten a patient's life expectancy, but may lead to uneasiness and panic, especially during social interactions.
ATLANTA (AP) — Allergy season can be miserable for tens of millions of Americans when trees, grass, and other pollens cause runny noses, itchy eyes, coughing and sneezing.
Where you live, what you’re allergic to and your lifestyle can make a big difference when it comes to the severity of your allergies. Experts say climate change is leading to longer and more intense allergy seasons, but also point out that treatments for seasonal allergies have become more effective over the last decade.
Here are some tips from experts to keep allergy symptoms at bay — maybe even enough to allow you to enjoy the outdoors.
The Asthma and Allergy Foundation of America issues an annual ranking of the most challenging cities to live in if you have allergies, based on over-the-counter medicine use, pollen counts and the number of available allergy specialists.
This year, the top five cities are: Boise, Idaho; San Diego; Tulsa, Oklahoma; Provo, Utah; and Rochester, New York.
Pollen is the powdery substance made by seed-producing plants and trees that is part of their reproductive process. Earlier in the spring, tree pollen is the main culprit. After that grasses pollinate, followed by weeds in the late summer and early fall.
Some of the most common tree pollens that cause allergies include birch, cedar, cottonwood, maple, elm, oak and walnut, according to the Asthma and Allergy Foundation of America. Grasses that cause symptoms include Bermuda, Johnson, rye and Kentucky bluegrass.
Pollen trackers can help you decide when to go outside. The American Academy of Allergy Asthma and Immunology tracks levels through a network of counting stations across the U.S. Counts are available at its website and via email.
The best and first step to controlling allergies is avoiding exposure. Keep the windows in your car and your home closed, even when it’s nice outside.
If you go outside, wearing long sleeves can keep pollen off your skin to help ward off allergic reactions, said Dr. James Baker, an allergist at the University of Michigan. It also provides some sun protection, he added.
When you get home, change your clothes and shower daily to ensure all the pollen is off of you — including your hair. If you can’t wash your hair every day, try covering it when you go outside with a hat or scarf. Don’t get in the bed with your outside clothes on, because the pollen will follow.
It's also useful to rinse your eyes and nose with saline to remove any pollen, experts said. And the same masks that got us through the pandemic can protect you from allergies — though they won’t help with eye symptoms.
Over-the-counter nasal sprays are among the most effective treatments for seasonal allergies, experts said.
But patients often use them incorrectly, irritating parts of the nose, said Dr. Kathleen May, an allergist at Augusta University in Georgia. She suggested angling the nozzle outward toward your ear rather than sticking it straight up your nose.
Over-the-counter allergy pills like Claritin, Allegra and Zyrtec are helpful, but may not be as effective as quickly since they're taken by mouth, experts said.
If your allergy symptoms are impacting your quality of life, like causing you to lose sleep or loose focus at work or school, it might be time to consider making an appointment with an allergist. There are medications that can train you immune system not to overreact to allergens.
Some remedies for allergy relief that have been circulating on social media or suggested by celebrities — like incorporating local honey into your diet to expose yourself to pollen — have been debunked.
Dr. Shyam Joshi, an allergist at Oregon Health and Science University, said that's because the flowers that bees pollinate typically don't contain the airborne pollen that causes allergy symptoms.
Winters are milder and growing seasons are longer as the climate is changing, meaning there’s more opportunity for pollen to stay in the air, resulting in longer and more severe allergy seasons.
Last year was one of the most intense allergy seasons on record, particularly in the Southeast U.S.
A version of this story was published April 19, 2025. The writer is no longer with The Associated Press.
The Associated Press Health and Science Department receives support from the Howard Hughes Medical Institute’s Science and Educational Media Group and the Robert Wood Johnson Foundation. The AP is solely responsible for all content.

FILE - Elena Ivanov, visiting from San Jose, Calif., walks across a field covered with blooming poppies near the Antelope Valley California Poppy Reserve in Lancaster, Calif., March 30, 2022. (AP Photo/Jae C. Hong, File)














