A research team from the Department of Orthopaedics and Traumatology, School of Clinical Medicine, LKS Faculty of Medicine of the University of Hong Kong (HKUMed), has demonstrated that robotic total hip replacement has a lower reoperation rate than the conventional technique. The study found a 90-day reoperation rate of only 0.6% with robotic procedures as compared to 2.5% with conventional procedures. Robotic procedures thus promise long-term benefits for patients, enabling them to regain mobility and return to normal life.
End-stage hip arthritis causes severe groin pain, joint stiffness and functional deficit, including impairment in walking, sitting and standing. While total hip replacement is a common operation, complications can occur and may lead to reoperation and prolonged recovery times.
Compared to conventional technique, robotic hip replacement utilises three-dimensional computed tomography scans for precise preoperative planning of both acetabular and femoral components. During surgery, acetabular bone preparation and implant positioning are carried out under robotic arm guidance, allowing for precise control over bone removal and cup placement.
Dr Henry Fu Chun-him, Clinical Associate Professor and Chief of the Division of Joint Replacement Surgery, Department of Orthopaedics and Traumatology, School of Clinical Medicine, HKUMed, said, ‘The robotic arm allows the direction and depth of the acetabular cup placement to be executed in accordance with preoperative planning, achieving angular precision down to 2 degrees and depth accuracy within 2mm.’
The research team reviewed the results of 553 primary total hip replacement surgeries performed in Queen Mary Hospital and the Duchess of Kent Children's Hospital at Sandy Bay Joint Replacement Centre between 1 January 2019 and 31 December 2024. These included 311 robotic total hip replacements and 242 conventional total hip replacements. The rate of reoperation within 30 and 90 days after surgery was lower for the robotic total hip replacement.
Dr Fu added, ‘Early reoperations after total hip replacement are devastating. With robotics, the rate of reoperation at 90 days is only 0.6%.’ In cases requiring reoperation in the robotic group, all procedures were done in a closed manner without the need for surgical reopening. In contrast, the conventional group had a 2.5% reoperation rate due to periprosthetic fractures and wound infections, requiring surgical reopening and resulting in prolonged recovery times.
While robotic procedures were associated with an overall increase in operative time of 14 minutes, the team observed a clear learning-curve effect, with surgical times progressively approaching those of conventional manual procedures.
HKUMed Department of Orthopaedics and Traumatology was the first in Hong Kong to utilise robotic arm technology for joint replacement surgery in public hospitals, beginning in January 2019.
Dr Amy Cheung Yim-ling, Honorary Clinical Assistant Professor and Deputy Division Chief of the Division of Joint Replacement Surgery of the same department, said, ‘The utilisation of robotics for total hip replacement in Queen Mary Hospital and the Duchess of Kent Children' s Hospital at Sandy Bay has risen steadily from 32% in 2019 to 85% in 2025. In the local public sector, robotic procedures now account for 49% of total hip replacement surgeries.’

HKUMed study demonstrates that robotic total hip replacement has a lower reoperation rate than the conventional technique. The research team members include Dr Henry Fu Chun-him (right) and Dr Amy Cheung Yim-ling.
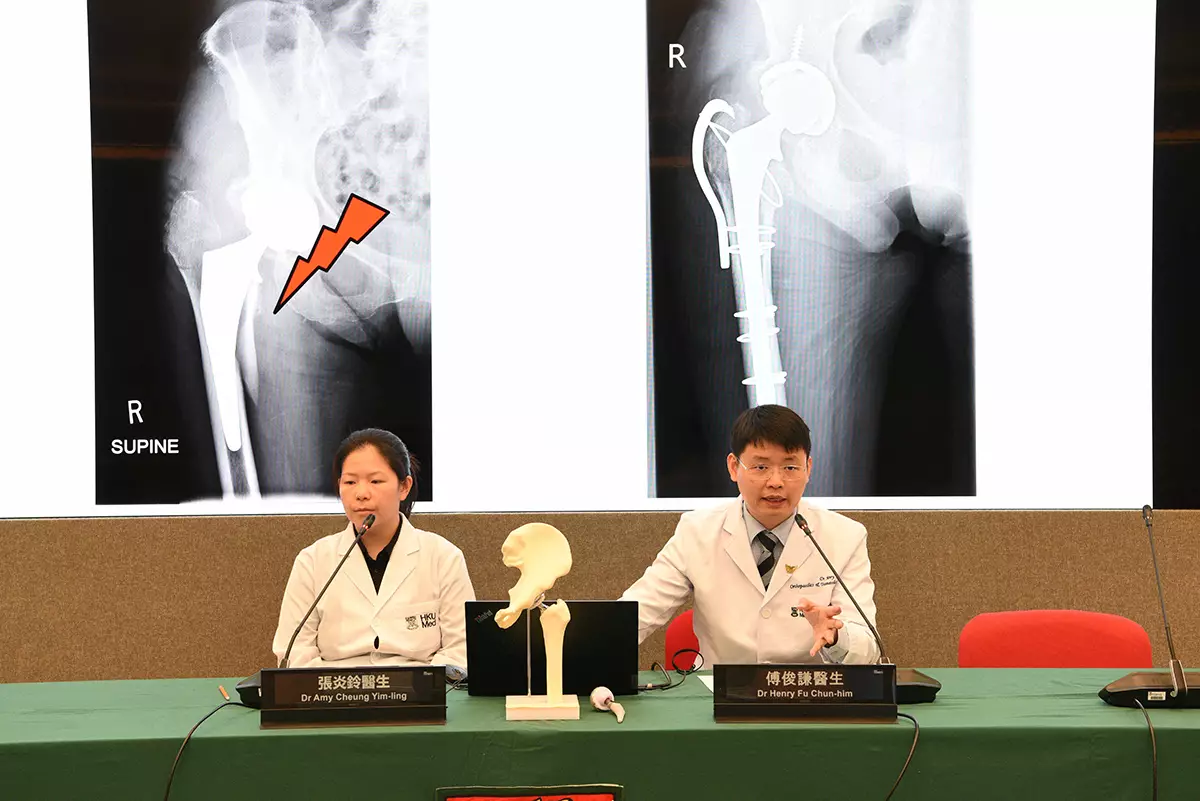
HKUMed study demonstrates that robotic total hip replacement has a lower reoperation rate than the conventional technique. The research team members include Dr Henry Fu Chun-him (right) and Dr Amy Cheung Yim-ling.

Dr Henry Fu Chun-him (right) highlights that increased experience has progressively shortened the surgery time of robotic total hip replacement. Ms Lai (middle), a patient who has recovered after the robotic surgery, shares that the robotic surgery helps her regain mobility and return to normal life.
A research team from the Department of Pharmacology and Pharmacy at the LKS Faculty of Medicine of the University of Hong Kong (HKUMed) has developed an innovative AI-based cardiovascular risk prediction tool, called CardiOmicScore. With a single blood test, the system can accurately forecast the future risk of six major cardiovascular diseases (CVDs): coronary artery disease, stroke, heart failure, atrial fibrillation, peripheral artery disease and venous thromboembolism. It can also provide early warning signals up to 15 years before clinical onset. The findings were published in Nature Communications [link to the publication].

HKUMed develops a cardiovascular risk prediction tool that can accurately predict the future risk of six major cardiovascular diseases with a single blood test. The system can provide early warning signals up to 15 years before clinical onset. The research is led by Professor Zhang Qingpeng (left).
AI-based multiomics integration reflects the body’s real-time health status
CVDs remain the leading cause of death worldwide, accounting approximately 19.8 million fatalities in 2022 alone. In routine health assessments, physicians typically evaluate cardiovascular risk based on age, blood pressure, smoking and other conventional clinical indicators. However, these measures often fail to capture subtle and early biological changes before the disease becomes clinically apparent, leading to many patients missing the optimal window for preventive intervention. Although polygenic risk scores have become popular in recent years, genetic predisposition is largely fixed at birth and does not change over time. Consequently, polygenic risk scores cannot reflect the immediate impact on health conditions resulting from lifestyle or environmental changes. This creates an urgent need for tools that can capture a person’s current biological state and provide accurate, early warnings for CVDs.
To address this problem, the HKUMed research team applied deep learning techniques to integrate multiomics data, including genomics, metabolomics and proteomics, to develop the CardiOmicScore tool. The study was based on large-scale population data from the UK Biobank, analysing 2,920 circulating proteins and 168 metabolites measured from blood samples. These molecular signals act as ‘real-time recorders’ of the body, sensitively reflecting subtle changes in the immune system, metabolism, and vascular health.
Professor Zhang Qingpeng, Associate Professor in the Department of Pharmacology and Pharmacy at HKUMed, explained, ‘Genes determine where we start—they define our baseline health risk. However, proteins and metabolites reflect our current physical health. Our AI tool is designed to decode these complex molecular signals, enabling doctors and patients to identify risks much earlier, which can potentially change the trajectory of disease through timely lifestyle modifications and early prevention.’
Accurate prediction of six major cardiovascular diseases with 15-year advance warning in high-risk groups
The results showed that CardiOmicScore transforms complex multiomics measurements into personalised risk scores with substantially improved predictive performance compared with conventional polygenic risk scores. When combined with clinical information such as age and gender, the model significantly enhanced the risk prediction accuracy of six common CVDs and can even flag elevated risk up to 15 years before symptoms appear.
This study marks a shift in precision medicine from a static, gene-centric paradigm towards a more dynamic, multiomics-based approach. In the future, a small-volume blood sample may be sufficient to generate a comprehensive cardiovascular risk profile for multiple diseases.
Professor Zhang added, ‘We aim to leverage technology to identify and prevent diseases before they develop. By shifting health management from reactive treatment to proactive prediction and intervention, we aim to create a lasting impact for both public health and individual patient care.’
About the research team
The study was led by Professor Zhang Qingpeng, Associate Professor in the Department of Pharmacology and Pharmacy, HKUMed, and the HKU Musketeers Foundation Institute of Data Science (IDS). The first author is Luo Yan from the HKU IDS.